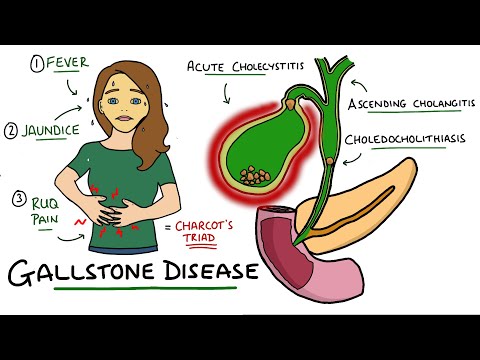
Choledocholithiasis⁚ An Overview
Choledocholithiasis refers to the presence of gallstones within the bile ducts, which can cause abdominal pain, jaundice, and impaired liver function. This condition requires prompt diagnosis and treatment to prevent complications such as pancreatitis.
Causes and Risk Factors
Choledocholithiasis is typically caused by the migration of gallstones from the gallbladder into the bile ducts. Several factors contribute to the formation of gallstones, including⁚
- Genetic predisposition
- Obesity
- Female sex
- Increasing age
- Familial history of gallstones
Additionally, certain medical conditions, such as diabetes, hypercholesterolemia, and liver disease, may also increase the risk of developing gallstones. Other risk factors include⁚
- Pregnancy
- Oral contraceptive use
- Ethnicity (e.g., Native American, Mexican-American)
- Dietary factors (e.g., high-fat diet)
Understanding the causes and risk factors associated with choledocholithiasis is essential for early detection and prevention of this condition.
Clinical Presentation
Patients with choledocholithiasis often present with symptoms of biliary colic, jaundice, and abdominal pain, which can be intermittent or persistent, and may be accompanied by signs of liver dysfunction or pancreatitis, requiring prompt medical evaluation.
Symptoms
The symptoms of choledocholithiasis can vary in severity and may include episodic or persistent abdominal pain, typically located in the right upper quadrant or epigastric region. Patients may also experience nausea, vomiting, and fever.
Jaundice is a common symptom, characterized by yellowing of the skin and sclera, and darkening of the urine. Some patients may also report pruritus, or itching sensations, particularly on the skin.
In some cases, patients may experience more severe symptoms, such as chills, rigors, and abdominal tenderness, which can indicate a more complicated course of the disease.
The frequency and duration of symptoms can vary widely among individuals, and some patients may remain asymptomatic for extended periods. However, it is essential to seek medical attention if symptoms persist or worsen over time.
A thorough evaluation of symptoms is crucial for an accurate diagnosis and effective treatment plan. A comprehensive clinical assessment should include a detailed medical history, physical examination, and diagnostic testing to confirm the presence of choledocholithiasis.
Physical Examination
A thorough physical examination is essential in the evaluation of patients with suspected choledocholithiasis. The examination should focus on the abdominal region, with particular attention to the right upper quadrant.
Patients may exhibit abdominal tenderness, guarding, or rebound tenderness, indicating inflammation of the gallbladder or bile ducts. A palpable mass or fullness in the right upper quadrant may be present, suggesting a distended gallbladder or bile duct obstruction.
The examiner should also assess for signs of jaundice, including yellowing of the skin and sclera, and darkening of the urine. Additionally, the patient’s vital signs, including temperature, pulse, and blood pressure, should be evaluated to detect any systemic signs of infection or inflammation.
A Murphy’s sign, which involves deep palpation of the right upper quadrant during inspiration, may be positive in patients with gallbladder disease. The physical examination findings should be carefully documented and considered in conjunction with laboratory and imaging studies to confirm the diagnosis of choledocholithiasis.
A thorough physical examination is crucial in determining the severity of the disease and guiding further management decisions.
Diagnostic Evaluation
A comprehensive diagnostic evaluation is necessary to confirm the presence of choledocholithiasis. This includes a combination of laboratory tests, imaging studies, and endoscopic procedures to visualize the bile ducts and detect gallstones.
Imaging Studies
Imaging studies play a crucial role in the diagnosis of choledocholithiasis. Several modalities are available, including⁚
- Ultrasound⁚ A non-invasive and widely available modality that can detect gallstones and bile duct dilation.
- MRI⁚ Provides detailed images of the bile ducts and surrounding structures, allowing for accurate detection of gallstones and other abnormalities.
- CT scan⁚ Can detect gallstones and bile duct dilation, as well as other conditions that may mimic choledocholithiasis.
These imaging studies can help identify the presence and location of gallstones, as well as any potential complications, such as bile duct obstruction or pancreatitis. A thorough interpretation of imaging results is essential for guiding further management and treatment decisions.
In some cases, imaging studies may not provide a definitive diagnosis, and additional testing or procedures may be necessary to confirm the presence of choledocholithiasis.
Endoscopic Retrograde Cholangiopancreatography (ERCP)
ERCP is a specialized procedure that combines endoscopy and fluoroscopy to diagnose and treat conditions affecting the bile and pancreatic ducts, including choledocholithiasis.
During an ERCP, a flexible tube with a camera and light on the end (endoscope) is inserted through the mouth and guided into the small intestine, where the bile and pancreatic ducts empty into the gut. A contrast agent is then injected into the ducts, allowing for visualization of the ductal system on X-ray.
ERCP is particularly useful in the diagnosis and treatment of choledocholithiasis, as it allows for⁚
- Direct visualization of the bile ducts and gallstones
- Removal of gallstones from the bile ducts
- Dilation of narrowed bile ducts
- Placement of stents to facilitate bile flow
ERCP is generally well-tolerated, but as with any invasive procedure, there are potential risks and complications, which should be carefully discussed with patients prior to the procedure.
Complications
Untreated choledocholithiasis can lead to severe complications, including pancreatitis, choledochal cysts, and biliary sepsis. Prompt diagnosis and treatment are essential to prevent these potentially life-threatening conditions and ensure optimal patient outcomes.
Pancreatitis
Pancreatitis is a serious complication of choledocholithiasis, occurring when a gallstone blocks the pancreatic duct, causing inflammation of the pancreas. This can lead to severe abdominal pain, nausea, vomiting, and potentially life-threatening complications.
The risk of pancreatitis is increased in patients with choledocholithiasis due to the proximity of the bile ducts to the pancreatic duct. If a gallstone becomes lodged in the common bile duct, it can obstruct the flow of pancreatic enzymes, leading to pancreatitis.
Pancreatitis associated with choledocholithiasis requires prompt medical attention, typically involving hospitalization and aggressive treatment to manage symptoms and prevent further complications. Endoscopic retrograde cholangiopancreatography (ERCP) may be necessary to remove the obstructing gallstone and restore pancreatic duct patency.
In severe cases, pancreatitis can lead to necrosis, organ failure, and death. Therefore, early recognition and treatment of choledocholithiasis are crucial to preventing this potentially devastating complication. A high index of suspicion and prompt intervention can significantly improve patient outcomes.
Choledochal Cysts
Choledochal cysts are congenital anomalies of the bile ducts that can increase the risk of developing choledocholithiasis. These cysts are characterized by dilatations of the bile ducts, which can lead to stasis of bile and formation of gallstones.
Choledochal cysts are often asymptomatic, but can cause symptoms such as abdominal pain, jaundice, and cholangitis if they become complicated by gallstones or other factors. In some cases, choledochal cysts can be associated with an increased risk of malignancy, particularly cholangiocarcinoma.
The presence of choledochal cysts can complicate the management of choledocholithiasis, as these cysts may need to be addressed surgically or endoscopically to prevent ongoing biliary obstruction and stone formation. In some cases, complete surgical excision of the cyst may be necessary to prevent long-term complications.
Early recognition and treatment of choledochal cysts are essential to preventing complications and improving patient outcomes. Imaging studies, such as ultrasound, CT, and MRI, play a crucial role in diagnosing choledochal cysts and guiding management decisions.
A multidisciplinary approach, involving gastroenterologists, surgeons, and radiologists, is often necessary to manage choledochal cysts and associated choledocholithiasis effectively.
Treatment
The primary goal of treatment for choledocholithiasis is to remove the gallstones from the bile ducts and restore normal biliary drainage. Endoscopic retrograde cholangiopancreatography (ERCP) with sphincterotomy and stone extraction is the preferred treatment modality.
In some cases, surgical intervention may be necessary, particularly if ERCP is unsuccessful or if there are multiple or large stones. Open or laparoscopic common bile duct exploration may be performed to remove the stones.
For patients with recurrent choledocholithiasis, cholecystectomy may be considered to prevent future episodes of gallstone formation. In addition, medical therapy, such as ursodiol, may be prescribed to dissolve small cholesterol stones.
Antibiotics are often administered prophylactically to prevent cholangitis and sepsis. Pain management is also crucial, and analgesics and anti-inflammatory medications may be prescribed to control symptoms.
A follow-up imaging study, such as ultrasound or CT, is typically performed to ensure complete clearance of the bile ducts and to rule out any complications. A multidisciplinary approach, involving gastroenterologists, surgeons, and radiologists, is often necessary to manage choledocholithiasis effectively.