Introduction to Trigger Finger
Trigger finger, also known as stenosing tenosynovitis, is a common condition characterized by finger stiffness, thumb pain, and tendon sheath inflammation, often resulting from repetitive strain injury, affecting individuals who perform repetitive activities.
1.1 Definition and Prevalence of Trigger Finger
Trigger finger, also referred to as stenosing tenosynovitis, is a condition characterized by the narrowing of the tendon sheath, leading to inflammation and constriction of the tendons. This results in a clicking or snapping sensation, accompanied by pain and stiffness in the affected finger or thumb.
The prevalence of trigger finger is estimated to be approximately 2-3% in the general population٫ with a higher incidence among individuals between the ages of 40 and 60 years. Women are more commonly affected than men٫ and the condition is often seen in individuals who engage in repetitive activities٫ such as typing٫ gripping٫ or grasping. The ring finger and thumb are the most commonly affected digits٫ accounting for approximately 75% of all cases. Trigger finger can significantly impact daily activities٫ causing discomfort٫ pain٫ and decreased dexterity.
A thorough understanding of the definition and prevalence of trigger finger is essential for early diagnosis and effective management of the condition.
1.2 Causes and Risk Factors of Trigger Finger
Trigger finger is often caused by repetitive strain or overuse of the tendons, leading to inflammation and narrowing of the tendon sheath. This can occur due to various factors, including repetitive grasping or gripping, forceful bending or straightening of the fingers, and prolonged use of vibrating tools.
Certain medical conditions, such as diabetes, rheumatoid arthritis, and gout, can also increase the risk of developing trigger finger. Additionally, individuals with a history of previous hand injuries or surgeries may be more susceptible to the condition.
Other risk factors for trigger finger include age, with the condition being more common among individuals over 40 years, and occupation, with certain professions, such as musicians, craftsmen, and industrial workers, being at higher risk due to the repetitive nature of their work. Furthermore, underlying conditions, such as tendonitis and tenosynovitis, can also contribute to the development of trigger finger.
Symptoms of Trigger Finger
Symptoms of trigger finger include finger stiffness, thumb pain, and a characteristic “catching” or “locking” sensation when flexing or extending the affected finger, often accompanied by tendon sheath inflammation and swelling.
2.1 Finger Stiffness and Locking
Finger stiffness and locking are hallmark symptoms of trigger finger, resulting from inflammation and narrowing of the tendon sheath. As the tendon becomes inflamed, it can no longer glide smoothly through the sheath, leading to a “catching” or “locking” sensation when attempting to flex or extend the affected finger.
This stiffness may be more pronounced in the morning, improving throughout the day as the finger is used. However, as the condition progresses, the stiffness can become persistent, making everyday activities increasingly challenging.
In severe cases, the finger may lock in place, requiring manual manipulation to release it. This recurrent locking can lead to pain, swelling, and further inflammation, exacerbating the condition and necessitating medical attention to prevent long-term complications and damage to the affected tendon and surrounding tissue.
2.2 Thumb Pain and Tenderness
Thumb pain and tenderness are common complaints among individuals affected by trigger finger, particularly those who experience triggering in the thumb. This pain can manifest as a dull ache or a sharp, stabbing sensation, often radiating from the base of the thumb to the palmar surface.
The pain may be exacerbated by activities that involve grasping, gripping, or pinching, such as writing, typing, or using tools. Tenderness can also be elicited by applying pressure to the affected area, which may be accompanied by swelling and erythema.
In some cases, the pain can be referred to the wrist or forearm, making it essential to conduct a thorough examination to determine the underlying cause of symptoms. A comprehensive evaluation will help clinicians distinguish thumb pain associated with trigger finger from other conditions, such as osteoarthritis or De Quervain’s tenosynovitis, to provide accurate diagnosis and targeted treatment.
2.3 Other Symptoms and Complications
In addition to finger stiffness, locking, and thumb pain, individuals with trigger finger may experience a range of other symptoms and complications. These can include a palpable nodule or thickening of the affected tendon, which can be tender to the touch.
Some people may also report a clicking or snapping sensation as the tendon moves through the pulley system, which can be audible in some cases. Morning stiffness, similar to that experienced by individuals with rheumatoid arthritis, is also common.
If left untreated, trigger finger can lead to complications such as persistent pain, limited mobility, and decreased grip strength. In severe cases, the condition can cause contracture of the affected finger, leading to permanent deformity. Furthermore, individuals with trigger finger may experience emotional distress and impaired quality of life due to the impact of symptoms on daily activities and overall well-being.
Diagnosis and Treatment of Trigger Finger
Accurate diagnosis and effective treatment of trigger finger require a comprehensive approach, incorporating medical history, physical examination, imaging studies, and various therapeutic options to address stenosis of tendons and alleviate symptoms.
3.1 Medical History and Physical Examination
A thorough medical history and physical examination are essential components of the diagnostic process for trigger finger. During the medical history, patients should provide detailed information regarding the onset and duration of symptoms, as well as any factors that exacerbate or alleviate the condition.
The physical examination typically involves a visual inspection of the affected finger, followed by a series of manual assessments to evaluate range of motion, tenderness, and crepitus. The examiner may also palpate the tendon sheath to assess for thickening or nodularity.
Additionally, the examiner may use various provocative maneuvers to reproduce the patient’s symptoms, such as flexion or extension of the affected finger. A comprehensive medical history and physical examination can provide valuable insights into the underlying causes of trigger finger and inform the development of an effective treatment plan.
By careful observation and manual assessment, healthcare professionals can accurately diagnose trigger finger and initiate timely interventions to address the condition and prevent further complications.
3.2 Imaging Studies and Diagnostic Tests
Imaging studies and diagnostic tests can be employed to confirm the diagnosis of trigger finger and rule out other potential causes of symptoms. Radiographs, such as X-rays, are typically used to evaluate for underlying bony abnormalities or fractures.
Ultrasound and magnetic resonance imaging (MRI) may be utilized to assess the tendon sheath and surrounding soft tissues, providing valuable information regarding tendonitis, tenosynovitis, or other inflammatory conditions.
Electrophysiological studies, including electromyography (EMG) and nerve conduction studies (NCS), may be performed to evaluate for potential neurologic compromise or compression neuropathy. Laboratory tests, such as erythrocyte sedimentation rate (ESR) or C-reactive protein (CRP), may be ordered to assess for underlying systemic inflammatory conditions.
While imaging studies and diagnostic tests can provide valuable information, they are often not necessary to diagnose trigger finger, as a thorough medical history and physical examination are typically sufficient to establish an accurate diagnosis.
3.3 Conservative Treatment Options
Conservative treatment options are often the initial approach for managing trigger finger, with the goal of reducing symptoms and improving function. Nonsteroidal anti-inflammatory medications (NSAIDs) may be prescribed to alleviate pain and inflammation.
Physical therapy, including exercises and stretches, can help maintain finger mobility and strength. Occupational therapy may also be beneficial in modifying daily activities and work-related tasks to reduce repetitive strain on the affected finger.
Steroid injections into the tendon sheath can be effective in reducing inflammation and relieving symptoms. Orthotics, such as finger splints or tape, may be used to immobilize the affected finger and reduce stress on the tendon sheath.
Modification of activities, rest, and ice may also be recommended to alleviate symptoms. Conservative treatment options are typically successful in managing trigger finger, with most individuals experiencing significant improvement or resolution of symptoms within several weeks to months.
3.4 Surgical Treatment Options
Surgical intervention may be necessary for individuals with trigger finger who have not responded to conservative treatment or have severe symptoms that interfere with daily activities.
The primary surgical procedure for trigger finger is a percutaneous release, which involves using a needle to release the constricted tendon sheath. This procedure is typically performed under local anesthesia and has a high success rate.
An open release surgical procedure may also be performed, which involves making a small incision to access the tendon sheath. This procedure allows for visualization of the affected area and is often used for more complex cases.
Both surgical procedures aim to relieve stenosis of tendons, restore normal tendon gliding, and alleviate symptoms. Post-operative rehabilitation may include physical therapy to maintain finger mobility and strength. Surgical treatment options can provide long-term relief from trigger finger symptoms and improve overall hand function.
Complications from surgery are rare, but may include infection, nerve damage, or recurrence of symptoms.
Prevention and Management of Trigger Finger
Effective prevention and management strategies for trigger finger include adopting ergonomic practices, taking regular breaks, and maintaining proper hand positioning to reduce repetitive strain and alleviate finger tendonitis symptoms.
4.1 Preventing Trigger Finger
Preventing trigger finger requires a proactive approach to reducing the risk of developing this condition. This can be achieved by adopting ergonomic practices in daily activities, particularly in occupations that involve repetitive hand movements. Proper hand positioning and alignment during tasks can also help minimize strain on the tendons and tendon sheaths.
Individuals who engage in activities that involve repetitive gripping, grasping, or twisting should take regular breaks to rest their hands and fingers. Stretching exercises can also help maintain flexibility and reduce the risk of stenosis of tendons. Furthermore, maintaining a healthy weight and managing underlying medical conditions, such as diabetes and rheumatoid arthritis, can also help prevent trigger finger. By taking these preventive measures, individuals can significantly reduce their risk of developing trigger finger and avoid the associated symptoms and complications.
4.2 Managing Trigger Finger
Effective management of trigger finger is crucial to alleviate symptoms, prevent progression, and improve quality of life. Individuals with trigger finger should prioritize activities that do not exacerbate the condition, such as avoiding repetitive gripping or grasping motions.
A home exercise program can be beneficial in managing trigger finger, focusing on gentle stretching and strengthening exercises for the affected fingers and thumb. Applying ice packs or heat therapy to the affected area can also help reduce pain and inflammation. Additionally, individuals can consider using assistive devices, such as ergonomic utensils or grips, to reduce strain on the affected fingers and thumb. By adopting these strategies, individuals with trigger finger can manage their symptoms, slow disease progression, and optimize functional ability. Regular follow-up appointments with a healthcare professional are also essential to monitor the condition and adjust management strategies as needed.
Conclusion
In conclusion, trigger finger is a complex condition that requires comprehensive understanding and management. By recognizing the definition, prevalence, causes, and risk factors of trigger finger, individuals can take proactive steps to prevent its onset.
A timely diagnosis and implementation of evidence-based treatment options can significantly improve outcomes for individuals with trigger finger. Furthermore, adopting strategies for prevention and management can reduce the risk of complications and optimize functional ability. It is essential for healthcare professionals to stay updated on the latest research and guidelines to provide optimal care for individuals with trigger finger. Ultimately, a multidisciplinary approach that incorporates education, prevention, and treatment can effectively address the challenges posed by trigger finger and improve the quality of life for those affected. By working together, we can reduce the burden of trigger finger and promote optimal hand health and function.
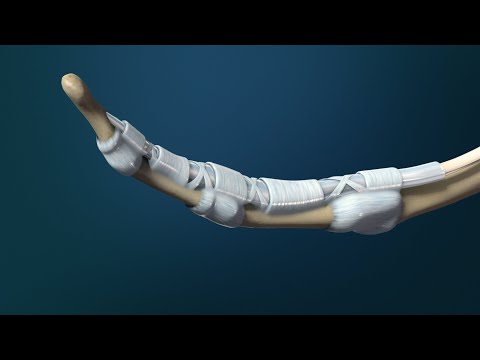
This article effectively raises awareness about trigger finger
The statistics provided on prevalence were interesting; however,a clearer explanation on how these numbers were derived would add credibility.
Overall well-written; however,a brief discussion on emerging treatments or research directions might provide readers with hope for future advancements.
I appreciate how this article highlights the importance of early diagnosis and effective management of trigger finger. The discussion on various treatment options would have been beneficial for readers seeking relief from this condition.
The connection between certain medical conditions like diabetes and rheumatoid arthritis with an increased risk for trigger finger was insightful.
The section on causes and risk factors was particularly informative, emphasizing the need for proper ergonomics in workplaces where repetitive strain injuries are common.
Including images or diagrams illustrating tendon sheath inflammation could enhance readers
This article provides a comprehensive overview of trigger finger, including its definition, prevalence, causes, and risk factors. The language used is clear and concise, making it accessible to both healthcare professionals and individuals affected by this condition.